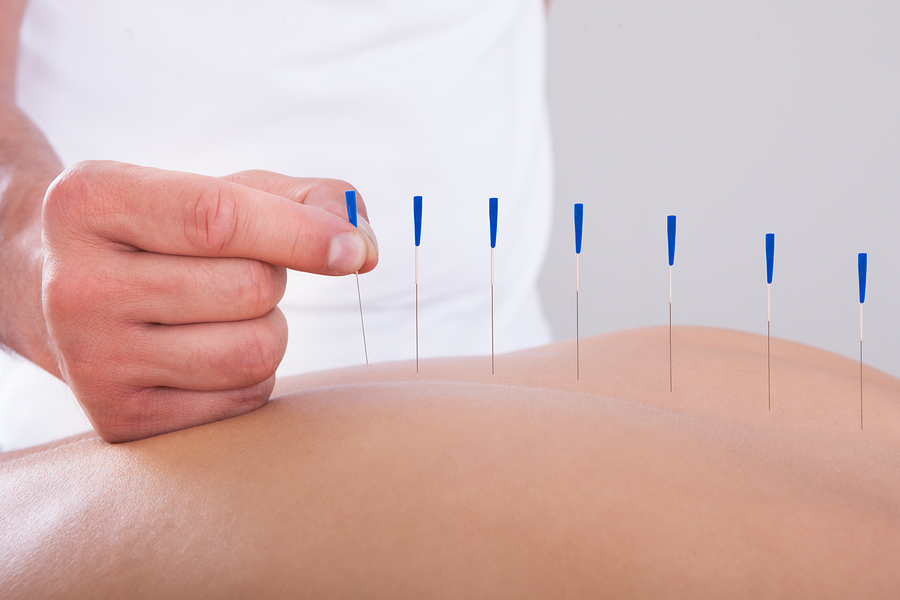
A needle-based technique has been shown to switch on nerves that tamp down sepsis (May 1, 2014 |By Gary Stix)
The ST36 Zusanli acupuncture point is located just below the knee joint. This spot in mice—and it is hoped perhaps in humans—may be a critical entryway to gaining control over the often fatal inflammatory reactions that accompany systemic infections. Sepsis kills as many as 250,000 patients in the U.S. every year, some 9 percent of overall deaths. Antibiotics can control sepsis-related infection, but no current drugs have fda approval for counteracting the runaway immune response.
Researchers at Rutgers University New Jersey Medical School reported online in Nature Medicine on February 23 that stimulating ST36 Zusanli with an electric current passed through an acupuncture needle activated two nerve tracts in mice that led to the production of a biochemical that quieted a sepsis like inflammatory reaction induced in mice. (Scientific American Mind is part of Nature Publishing Group.)
The finding, which also involved the collaboration of the National Medical Center Siglo XXI in Mexico City and other institutions, raises the possibility that knowledge derived from alternative medicine may provide a means of discovering new nerve pathways that can regulate a variety of immune disorders, from rheumatoid arthritis to Crohn’s disease. If future studies achieve similar results, acupuncture might be integrated into the nascent field of bioelectronics medicine—also called electroceuticals—that is generating intense interest among both academics and drug companies.
Clues from Acupuncture
Luis Ulloa, who headed the study at the Center for Immunity and Inflammation at Rutgers, has spent more than 10 years researching how nerve signals control immune function. Following the suggestion of a Mexican colleague, he realized that it might be worth testing whether acupuncture could help discover some of these much sought neuroimmune pathways.
Ulloa and his team used electroacupuncture to stimulate the ST36 Zusanli acupuncture point in 20 mice exposed to lipids and carbohydrates from the outer membrane of bacteria, producing an inflammatory response that mimics sepsis. Another 20 rodents received “sham” electroacupuncture in which nonacupuncture points were stimulated. Half of the mice in the first group survived, whereas all the sham-treated rodents perished. A similar survival difference was noted with two groups of mice exposed to a cocktail of microbes in the gut.
Researchers then began to analyze the nerves and organs involved. They traced a pathway beginning in a branch of the sciatic nerve, not far from ST36 Zusanli, that relayed a signal to the spinal cord and then the brain. Once processed there, it was sent down to the vagus nerve, finally reaching the adrenal glands, which produced the key anti-inflammatory agent, the neurotransmitter dopamine. Ulloa’s team set about confirming the parts of this biological wiring diagram by removing independently sections of the key nerves and the entire adrenal glands. Excision of any one of these links in this newly discovered neuroimmune circuit abolished electroacupuncture’s anti-inflammatory effects.
The researchers also succeeded in quelling inflammation by using a drug called fenoldopam (Corlopam), which acted as a stand-in for the adrenal-produced dopamine in mice who had the glands surgically removed. Having a drug at hand might be essential because the adrenals in many sepsis patients function poorly, which makes them unsuitable candidates for acupuncture therapy.
The Rutgers work with acupuncture might be a relatively noninvasive means of performing neuroimmune stimulation and researching the interaction between the nervous and immune systems. “There are hundreds of these [neuroimmune] circuits that haven’t been mapped, and some of them may map to acupuncture points,” says Kevin Tracey of the Feinstein Institute for Medical Research on Long Island, who is one of the pioneers of bioelectronic medicine.
Tracey, a former colleague of Ulloa’s, adds that studies such as the one from the Rutgers group could help establish a physiological mechanism to explain why acupuncture might work as a treatment. Tracey’s own research led to the founding of a company called SetPoint Medical in Valencia, Calif., which is developing an implantable device to activate a separate neuroimmune pathway to treat inflammatory diseases.
Testing Ancient Treatments
Acupuncture still has its critics at various ends of the medical spectrum. Some acupuncture proponents perceive a study on sepsis as a case of Western medicine finally conferring a belated blessing on techniques that have been accepted treatments for thousands of years. Skeptics of alternative medicine, meanwhile, criticize any investigation of acupuncture as a waste of limited research dollars on a folk remedy for which a firm scientific basis will never be found.
Steven Novella, president of the New England Skeptical Society, characterizes the sepsis study as having merely shown that a nerve responds to the application of an electric current. “Electroacupuncture itself is not a real entity, in my opinion,” he says. “It is just electrical stimulation. Doing stimulation through an ‘acupuncture needle’ is meaningless—it’s just a thin needle. There’s nothing that makes it an acupuncture needle. And there is no evidence that acupuncture points exist at all.”
For his part, Ulloa had no intention of trying to determine whether flows of vital energy, or qi, were making their way through the body’s “meridians” based on the interpretation for how acupuncture works in Chinese traditional medicine. In fact, he agrees with Novella’s argument about nerve stimulation. In the study, the researchers found no anti-inflammatory effect when a toothpick was used to probe ST36 Zusanli, in a manner similar to the way acupuncture needles had been inserted for centuries before the advent of electroacupuncture.
As a prospector for neuroimmune pathways, Ulloa insists his interest in exploring acupoints in his research has not flagged. “It is no coincidence that all acupoints but one—360 of 361 described in humans—are located in the proximity of a major nerve,” Ulloa says. In his study, ST36 Zusanli led directly to the discovery of one of the most intricate neuroimmune circuits found to date. “Instead of testing millions of potential points, we reasoned that acupoints may provide an advantage in stimulating neuronal networks more efficiently,” he says.
A few days after the acupuncture paper in Nature Medicine appeared, a study published in Science Translational Medicine documented that a component of the herb Salvia miltiorrhiza, another hand-me-down from the Chinese traditional medicine pharmacopeia, also turned out to have potent anti-inflammatory properties. The researchers from leading institutions who wrote that paper were taking the same path as Ulloa and his team, attempting to test whether an ancient treatment had through trial and error turned up some biological effect or therapeutic potential that could be subject to a rigorous testing regimen in the laboratory.
In both reports, the authors were following the dictates that top-flight journal editors, article reviewers—and the skeptics themselves—endorse for evidence-based medicine. This type of study will certainly be more the exception than the rule. These same journals will never be publishing on feng shui and homeopathy—and the acupuncture entries in their pages will still be relatively scarce. But if scientists studying acupuncture or herbs can cross the high bars set by the scientific establishment, what’s wrong with that?